The Complete Varicose Eczema Treatment Guide
Varicose Eczema, also known as venous eczema or stasis dermatitis, is a medical condition which describes the dry irritated skin caused by abnormal pressure in the leg veins. Varicose eczema occurs in the legs and is more common in people with varicose veins. However, varicose veins do not have to be present to have varicose eczema.
Symptoms of Varicose Eczema
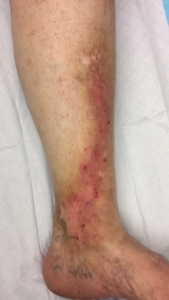
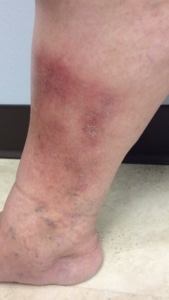
- Patients have patchy areas of dry, flaky, itchy skin on the lower legs. The itching can lead to scratching or skin break down.
- These areas of dry skin can crack and bleed or blister. In severe cases, the skin can ulcerate. Skin ulcers in patients with venous insufficiency can take months to heal.
- The skin can have a brownish discoloration. The texture of the discolored skin is often different from the rest of the leg.
- Symptoms can improve and worsen over time. Although, without treating the underlying problem, the symptoms will always recur.
What Causes Varicose Eczema?
Patients with venous insufficiency have abnormal function of the valves in their veins. These valves protect against the backward flow of blood in the vein. Without functioning valves, standing causes sudden pressure changes in the veins. This sudden pressure change causes the veins to enlarge and leak. Subsequently, the body responds to the small leak. This response causes local inflammation. Eventually, the inflammation can cause the skin changes that leads to varicose eczema.
How is Varicose Eczema Diagnosed?
To diagnose varicose eczema a sonographer performs an ultrasound. Usually, the sonographer positions the patient in standing or legs down position. Generally, there is no flow in the lower leg veins at rest. The technologist squeezes the lower leg and watches for blood flow to move towards the heart. Then, they watch the valves in the veins to see if there is a backwards flow. The backwards flow can be from a valve problem. The video below demonstrates imaging of a vein during the ultrasound examination. Initially, there is a surge of blue in the vein. The blue is the blood moving towards the heart after the sonographer squeezes the leg. Subsequently, the red color is the backwards flow of blood in the leg or the venous insufficiency.
How is Varicose Eczema Treated?
Initial management is with conservative care including:
-
Maintaining a healthy weight
-
Exercise: Walking and while sitting, heel -toe- maneuvers or toe crunches. Any contraction of the calf muscle will propel the blood in the legs toward the heart. The calf muscle pump is important to keep the blood from pooling in the legs.
-
Compression stockings: Medical grade graduated compression stockings are tightest at the ankle. The level of tightness decreases as they go up the leg. Thereby, pushing the fluid in the legs upward against gravity. We recommend wearing compression stockings during the day time. We especially recommend compression stockings for periods of prolonged standing, sitting or travel. Compression stockings are not needed at night while sleeping. At night, the feet are elevated to heart level.
-
Topical skin treatments: Applying moisturizers to the skin keeps the skin from becoming dry. The better moisturizers are thick and do not easily pool in the cap when the jar or tube is turned over. Topical steroid creams can help reduce the inflammation and itching.
Varicose Eczema Treatment: Procedures
Vein treatments are often needed if conservative management fails. Procedures treat the underlying cause of the venous insufficiency. There are many treatments for venous insufficiency all with advantages and disadvantages. Look for a physician who offers many kinds of treatments to treat your unique anatomy.
Superficial venous insufficiency the treatments can include:
-
Laser vein ablation: The physician advances a small laser into the abnormal vein. The physician then places fluid and numbing medication around the vein. The fluid and numbing medication has three purposes. It insulates the surrounding tissues, compresses the vein on the laser and numbs the area. The laser, which is a heat source sears the abnormal vessel closed. The physician uses ultrasound to guide the procedure. Over time, your body absorbs the vessel.
-
Radiofrequency vein ablation: Radiofrequency vein ablation works like laser vein ablation. The probe is a heat source which sears the vessel closed. Both laser and radiofrequency ablation have slightly different advantages.
-
Chemical vein ablation: Specialized polidocanol foam. The medication is a detergent which destroys the lining of the vessel. The physician places the medication through a needle or small catheter (tube) directly into the abnormal vein.
-
Mechanico-chemical vein ablation: Usually under trade name of Clarivein. Clarivein uses a combination of a mechanical wire and a medication to destroy the lining of the vein.
-
Venaseal: A sterile, surgical glue seals closed the abnormal vein. The advantage is that there is no required stocking use after the procedure.
-
Microphlebectomy: Removing the bulging varicose veins through a tiny nick in the skin. Removing the bulging veins through a nick the size of a ballpoint pen head is possible because there is no blood in the veins. It is like taking out a deflated balloon.
-
Sclerotherapy: Injection of a substance into the vein to close the veins. The FDA approved medications for sclerotherapy include polidocanol and sotradecol. Both medicines are detergents. Physicians can also use hypertonic saline, glycerine and other agents. It is important to discuss with your physician the medicines they plan to use, and any side effects.
Deep Venous Insufficiency Treatments:
Deep venous insufficiency can be more difficult to treat. The choice of treatment depends on the initial cause of the deep venous insufficiency. Different treatments exist for chronic deep venous thrombosis or outflow obstruction of the vein. Correct treatment requires consultation with a vascular or vein specialist. Treatments include:
-
Venous lysis. The physician gives a blood thinning medication into the vein slowly, in a hospital to open clotted vessels
-
Venous dilation and/or stenting . Primarily, physicians perform venous stenting in narrowed pelvic veins. The physician places a metal mesh stent across the narrowing. They may dilate the vessel with a balloon before or after stenting. The improved vessel diameter aids the movement of blood.
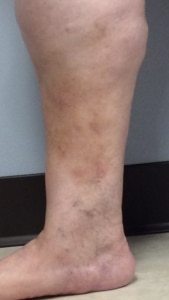
Before and After Pictures of Varicose Eczema
These are pictures of the lower leg of a Lakeshore Veins patient before and after treatment for superficial venous insufficiency. Her skin has healed. In addition, she is happy she no longer has the itching, bleeding, skin wounds.